
Fighting Cholera with Satellites and Smartphones
How a Moravian University economics professor hopes to use data from NASA to ease the suffering from waterborne disease in Bangladesh
By Jeff Csatari
Photographs by Kriston Jae Bethel
The parents brought their child to a field hospital at Matlab, Bangladesh. The 6-year-old girl looked like a cadaver. She was pale, drawn, and leathery-skinned from sudden dehydration and doubled over with cramps, suffering from the telltale symptom of cholera, a watery-grey diarrhea often described as rice-water diarrhea.
An off-season outbreak of the waterborne bacterium Vibrio cholerae had occurred, and the child was among patients streaming into the hospital from the surrounding villages. She was barely clinging to life. The doctors didn’t think she would make it through the night.
Cholera, caused by ingesting food or water contaminated by V. cholerae, triggers a violent, uncontrollable loss of body fluids through vomiting and diarrhea. In Bangladesh, there are two primary cholera seasons. During the spring dry season, seawater from brackish estuaries moves upstream into the low rivers and tributaries, bringing with it microscopic crustaceans called copepods that carry the cholera bacteria. The salty water and warm temperatures create the perfect environment for the algae that the copepods feed on and, as a result, the colonization of the cholera bacteria.
The second season occurs during the rainy fall after the monsoons, when cholera outbreaks are linked to flooding, which compromises sanitation systems and spreads fecal material containing V. cholerae into surface water. Because people use the rivers and other surface water for bathing, washing fruits and vegetables, and drinking, the pathogens are easily transmitted to humans. Cholera, the world’s longest ongoing pandemic, is one of the world’s most rapidly fatal illnesses. Without treatment, death occurs within 24 hours, sometimes in fewer than eight. In the 1970s, it was the leading cause of death in Bangladesh. The gold standard treatment is antibiotics and rehydration through intravenous fluids, but that’s expensive, so the preferred method in Bangladesh is an oral rehydration drink full of electrolytes—think Gatorade, but much cheaper—a solution developed by the International Centre for Diarrhoeal Disease Research, Bangladesh (ICDDR,B). An equivalent even cheaper household solution was also developed using water, sugar, salt, and molasses.


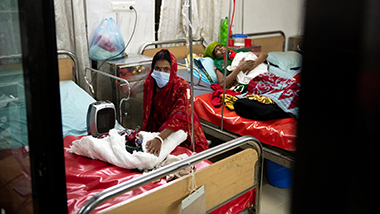
Above: Sonia Aziz, associate professor of economics, speaks with a cholera patient at a field hospital in Matlab, Bangladesh;
Aziz visits a village in Matlab; Infants are treated for cholera with IV fluids at the ICDDR, B Matlab field hospital.
Near death, the girl couldn’t keep down the rehydration solution given to her at Matlab Hospital. The medical staff tried desperately to find a viable vein to insert the IV tube for the saline drip she needed to survive.
Many victims do not survive. Depending on the severity of outbreaks, 1.3 to 4 million cases of cholera are reported annually, and 21,000 to 143,000 deaths occur worldwide, according to the World Health Organization (WHO). In Bangladesh alone, 66 million people are estimated to be at risk for cholera and more than 4,500 die each year.
Eight thousand miles from rural Matlab, Sonia Aziz, associate professor of economics at Moravian University, sits in her second-floor office in the Priscilla Payne Hurd Academic Complex poring over spreadsheets from her research, data derived from the interconnection of NASA satellites, smartphones, and households in the floating urban slums of Matlab.
“You can’t see cholera in a glass of water,” Aziz explains. “But NASA can see it from space.”

Women in rural Bangladesh wash cooking pots and utensils, clothes, and shoes in a pond.
Satellites in low Earth orbit can measure signs in large bodies of water that indicate environmental conditions are ripe for emerging cholera blooms. That knowledge can provide an early warning of the danger to vulnerable populations, who can then take preventive measures such as boiling drinking water, avoiding washing fruits and vegetables with untreated water, and getting a cholera vaccine. The early warning signal can be delivered to people on their cellular phones through a special app Aziz’s research team developed.
An environmental economist, Aziz’s mission is to determine if access to that warning signal changes behaviors of the people who are in harm’s way. In short, will the poor of Bangladesh use it? And does it save both lives and money? The cost of an episode of cholera can run as high as US$206 for hospitalization.



Above: A village woman collects water from a tube well in rural Bangladesh;
A Muslim child performs ritual washing prior to prayers at a mosque in Matlab; Aziz talks with villagers during her study in Matlab.
For Aziz, the calculations are much more than an intellectual challenge. They represent people—her people. Aziz was born in Dhaka, the capital city of Bangladesh, and raised there, though she has also lived in Oman and Saudi Arabia, where her father’s work took the family. Her father, KMS Aziz, PhD, is a world-renowned microbiologist. He studied at Duke University in North Carolina and then came back to Bangladesh to begin work, where he was instrumental in the development of an oral rehydration salt solution (ORS). In 1978 when the WHO launched a global diarrheal-diseases control program, Dr. Aziz began disseminating the ORS packets throughout Bangladesh. For his contributions to the field of Oral Rehydration Therapy (ORT) for diarrhea management, the American Association for the Advancement of Science elected him as a fellow in 1985.
While Sonia Aziz was a teenager, she often traveled with her father to rural areas where she witnessed people suffering from cholera and experienced several bouts with the disease herself—one so bad it required hospital care. “There’s no pleasant way to say this, but you lose so much liquid volume through a combination of vomiting and all other kinds of output,” she says. “It feels like you’re going to die.”
But once your body is rehydrated, you typically bounce back quickly. “It’s amazing; you are a completely different person after treatment,” says Aziz. Fortunately, the little girl in Matlab Hospital experienced the same speedy recovery once her body was rehydrated through the IV. The next day she sat up to play with dolls, smiling and giggling like a normal 6-year-old.

An urban pond in Dhaka, Bangladesh, is used as a dumping ground for garbage and for washing clothes.
Arsenic in Groundwater
Despite the early exposure to her father’s work, Aziz had no interest in becoming a scientist. “But I always had a good feeling for research organizations like ICDDR,B that would do these amazing things and bring about change,” she says.
Aziz, whose parents have homes in Bangladesh and the United States, chose the University of Texas at Austin to pursue an economics degree. In the early ’80s, she says, economics was very math oriented, very theoretical. “It wasn’t applied. It didn’t feel real to me.” So she did her postgrad work in environmental economics, which puts value on nonmarket goods like clean air and water. Given her background shadowing her father in his work, she began focusing on water quality. She attended the University of Maine, where faculty studied the hazards of arsenic in the state’s groundwater. Arsenic is a chemical element found naturally in soil and rock that can leach into well water. During her time in Maine, a large study exposed severe arsenic contamination in well water in Bangladesh.
In the second half of the century, the Bangladesh government began a nation-wide effort to switch water sources to shallow tube wells to quell the incidence of cholera from surface water. The campaign was hugely successful, but in the 1980s people using the wells started displaying skin lesions and cancers. Water testing revealed that those wells throughout Bangladesh tapped into aquifers contaminated with arsenic. The WHO has called that well-use program the largest mass poisoning in history.
For her dissertation, Aziz proposed a WHO-funded study to determine if people living in rural areas of Bangladesh would walk a longer distance to retrieve water from a well that had been painted green to indicate “safe” or take their chances with a more convenient well marked red for “unsafe, or arsenic tainted.”
“I gave Sonia free rein on her PhD,” says her dissertation advisor, Kevin Boyle at the University of Maine, now a professor of agricultural and applied economics at Virginia Tech University. “She was a student who came in with a real passion for doing research that would improve living conditions for people in Bangladesh who do not have the resources readily available to them.”
Ultimately, Aziz’s arsenic study was published; it found that people were willing to walk a substantial distance to access the safe drinking water. Boyle says the arsenic research naturally led her to take on the second major health issue related to water quality in Bangladesh—cholera.



Above: Drinking water stored in drums in urban slums; In the Matlab field lab,
a technician examines a petri dish for cholera caused by the bacterium Vibrio cholerae; Aziz interacts with a toddler in Matlab.
Aziz won two highly competitive research grants, one from NASA and another from the Valuables Consortium at Resources for the Future (RFF), a leader in economic analysis for managing natural resources. The studies focused on valuing information provided by NASA’s Earth-observing satellites. Boyle says Aziz put together a stellar team of expert engineers, computer scientists, and environmental economists for the grant applications.
The first grant funded a study looking to determine the viability and cost savings of using a satellite-derived early warning system to predict cholera outbreaks during the dry season and monsoon season when hospital patients overflow into the streets.
Cholera vaccines are about 60 percent effective at preventing illness, but they are expensive. “It’s not a sustainable solution for people who are poor,” says Aziz. (Two of every five Bangladeshis are officially classified as poor.) “And you still have to protect yourself by having a higher level of awareness and boiling your water during times of higher risk.”
Aziz’s study involved sending ambassadors into rural villages to survey households to determine if people would be interested in an early warning system. That data could then be used to estimate the potential medical cost savings of prevention, something that would be of keen interest to policymakers in the Bangladesh government.
The survey takers also asked women and girls—the primary arbiters of water safety decisions in households—by which mode they would prefer to receive an early warning of cholera outbreaks. “There was a high degree of receptivity to receiving the messages through a cell phone app,” says Aziz. (Even families living in bamboo shacks without sanitation have smartphones, their most useful connection to the outside word.) “We were surprised to find people were handing over their phones and saying, ‘Can you give it to us now?’
But an app had yet to be developed. Enter the RFF grant.
“We were surprised to find people were handing over their phones and saying, ‘Can you give it to us now?’”
—Sonia Aziz, associate professor of economics

Aziz travels on a traditional boat made of wood and bamboo to her field site in Matlab.
CholeraMap
Aziz is an economist, not an engineer or computer scientist, so she put together a team of experts as well as villagers in Bangladesh to collaborate on the design and development of the app, called CholeraMap. Her crew includes Ali S. Akanda, associate professor of civil and environmental engineering at the University of Rhode Island, Emily Lambright-Pakhtigian ’15, a former student of Aziz’s who is now assistant professor at the School of Public Policy at Penn State University, mentor Boyle as advisor, and S.M. Manzoor Ahmed Hanifi, a senior scientist at ICDDR,B.
Akanda developed the risk model based on environmental conditions gathered from the satellites that feeds that app. He tapped a computer science doctoral student at URI to build the code powering CholeraMap, which transmits that risk information to villagers’ smartphones. Pakhtigian, who helped Aziz with her arsenic work while an undergrad at Moravian, supervised the field research teams that surveyed villagers about the usefulness of the app.



Above: Crowded passageways are typical of slum dwellings in Dhaka; Patients sit in a waiting room at the Matlab field hospital awaiting treatment for cholera; Aziz at the Matlab field station.
“We won’t know until the analysis is done if [our work] will be something of use,
but it means a lot to be able to come back here, connect with my people, and do something that may help.”—Sonia Aziz
During the study, the researchers compared data from households using the app and those not using it. They tracked such metrics as cholera-related hospital visits, water-usage behaviors, cost of treatment, and lost productivity due to bouts of diarrheal disease. Pakhtigian, Boyle, and Aziz are still analyzing data, but preliminary data suggest that the app users have changed their behaviors, taking greater precautions during times of high risk.
The app displays a color-coded map of the local area with the users’ households geo-located on the smartphone: Green areas indicate low risk, yellow signals moderate risk, and red warns of high risk. The app’s graphics also show an animation of a Bangladeshi woman that provides easy-to-understand recommendations on what to do to prevent cholera: boiling drinking water, not swimming, and not rinsing vegetables in water that may be contaminated. The graphics were illustrated by Moravian graphic design student Anna Litofsky ’22.
“Another wonderful thing about Sonia is that she always tries to integrate academics with her research by getting undergrad students involved,” says Boyle. That’s exactly how Pakhtigian ultimately found her own place in research and teaching. “Sonia is a tenacious researcher with a tireless work ethic and curiosity to ask questions,” says Pakhtigian. “In the classroom, she sets really high standards; she pushes people to achieve much more than they think they can.”

Creating Opportunities for Students
Since beginning her work in Bangladesh, Sonia Aziz, associate professor of economics, has involved undergrads with her research.
Lowell Perkins ’17, Nathaniel Rhoads ’19, and Hannah Hook ’20 graduated from Moravian with honors for their thesis work in the prevention of cholera using a satellite-assisted early warning system. Perkins earned a PhD in economics from Clark University this year, and Hook will complete her master of science degree in infectious diseases in global health at Tufts University this August. Emily Lambright Pakhtigian ’15 is an assistant professor at the School of Public Policy at Penn State University.
Photo: Moravian alumna Hannah Hook ’20 visits a field site in Dhaka, Bangladesh
Aziz is in her happy place, sitting inside a mosquito tent in Matlab, chatting with someone from Moravian University in Bethlehem over a crystal-clear Zoom connection. “There are a lot of big bugs here,” she says. “But I’ve got one of those bug zappers that look like tennis rackets right next to my chair,” she adds with a laugh. Aziz is back in Bangladesh to meet with ICDDR,B and investigate additional variables that will help her prepare her research for publication. The results of her studies are mixed, she says, and still being analyzed, but she expects to show that providing households with a satellite-aided warning of cholera risk improves their decisions to take precautions. And she hopes that that knowledge—and its potential to save lives and money—will encourage policymakers to implement effective ways to limit the incidence and spread of cholera.
“We won’t know until the analysis is done if [our work] will be something of use, but it means a lot to be able to come back here, connect with my people, and do something that may help,” she says.
Aziz pauses, looking off screen for a few moments. “I have an emotional connection to the people here. I speak the language. And I think it is totally random that I was born to a family of privilege. I could have been anybody in rural Bangladesh. That’s something I grew up watching, and it has always struck me how random fate can be. Yes, it means the world to me to do this work.”
Jeff Csatari is executive editor of Galvanized Brands (the media company founded by David Zinczenko ’91) and an adjunct professor of journalism.

Aziz explains the CholeraMap smartphone app her research team
developed to provide an early warning system to prevent cholera.
Safe Water from Smartphones
CholeraMap, created by a team led by Moravian University economics professor Sonia Aziz, is an app that identifies cholera “hotspot” locations based on environmental data monitored by NASA satellites. Sensors on the satellites don’t detect the actual bacteria; they spot chlorophyll in the phytoplankton, also known as microalgae, that drifts on the surface of oceans and bodies of freshwater. Chlorophyll has a green pigment because it absorbs red and blue light and reflects green light, which satellite sensors can measure. Cholera bacteria live on copepods, microscopic zooplankton, which feed on phytoplankton. So, using chlorophyll as a marker, scientists can surmise that more chlorophyll means more food for copepods, which means more risk of cholera outbreak. Other environmental factors, such as sunlight, temperature, precipitation, and salinity, work into the equation that allows scientists to accurately predict high cholera risk up to two weeks in advance.
The CholeraMap app pinpoints the user’s geolocated household on a color-coded map. Green indicates the water is safe to drink, yellow means caution, and red warns of a high risk of cholera contamination. Another tab shows a cartoon graphic telling the story of a young woman receiving the risk notification. She’s wearing a salwar kameez and a concerned look on her face. Recommendations written in Bangla explain how to interpret the level of risk. A third tab is an animation illustrating boiling water, not swimming in contaminated water, washing fruits and vegetables with safe water, and other precautions. The illustrations were drawn by Moravian University art student Anna Litofsky ’22.
The app is user-friendly and very scalable, says Ali S. Akanda, the University of Rhode Island engineering professor who developed it. He believes it can be useful in other parts of the world, such as Africa, to track cholera and may someday be used as an early warning system for similar water-quality issues.

Screenshots from CholeraMap
To learn more about Resources for the Future and Aziz's work for the Consortium for the Valuation of Applications Benefits Linked to Earth Sciences, visit Grants for Assessing the Benefits of Satellites research at rff.org/valuables/gabs. —J.C.
